The American Medical Association has endorsed a resolution urging hospitals across the country to provide nutritious plant-based meal choices for patients, staff, and visitors.
Around the world, poor dietary habits contribute to approximately 11 million deaths each year, making unhealthy eating the top risk factor for mortality, surpassing all other causes. With diet standing as the primary driver of death globally, one might expect robust nutrition training to be a cornerstone of medical education and professional development. However, significant shortcomings persist in this area. A comprehensive analysis revealed that, despite nutrition’s pivotal role in maintaining wellness, final-year medical students often lack the preparation needed to deliver effective, evidence-based dietary guidance to those under their care.
This educational gap could be addressed even earlier, perhaps at the undergraduate level. Should aspiring doctors prioritize studying the world’s leading cause of death or delve deeply into subjects like organic chemistry?
During medical school, learners typically receive just about 19 hours of nutrition education amid thousands of hours dedicated to other topics, and much of that limited instruction fails to cover the most practical and relevant material. How often will physicians diagnose rare conditions like scurvy or beriberi, which stem from nutrient deficiencies? Far more frequently, they will treat patients grappling with the consequences of overconsumption-conditions such as obesity, type 2 diabetes, high blood pressure, and cardiovascular disease. These diet-related excesses are commonplace in everyday practice, unlike those deficiency diseases. Remarkably, 95% of cardiologists polled affirm that they should offer patients at least fundamental dietary advice, yet fewer than 10% consider themselves proficient experts in nutrition.
Clinical protocols for managing atherosclerotic cardiovascular disease-our foremost dietary killer-emphasize initiating treatment with wholesome lifestyle modifications, including dietary changes.
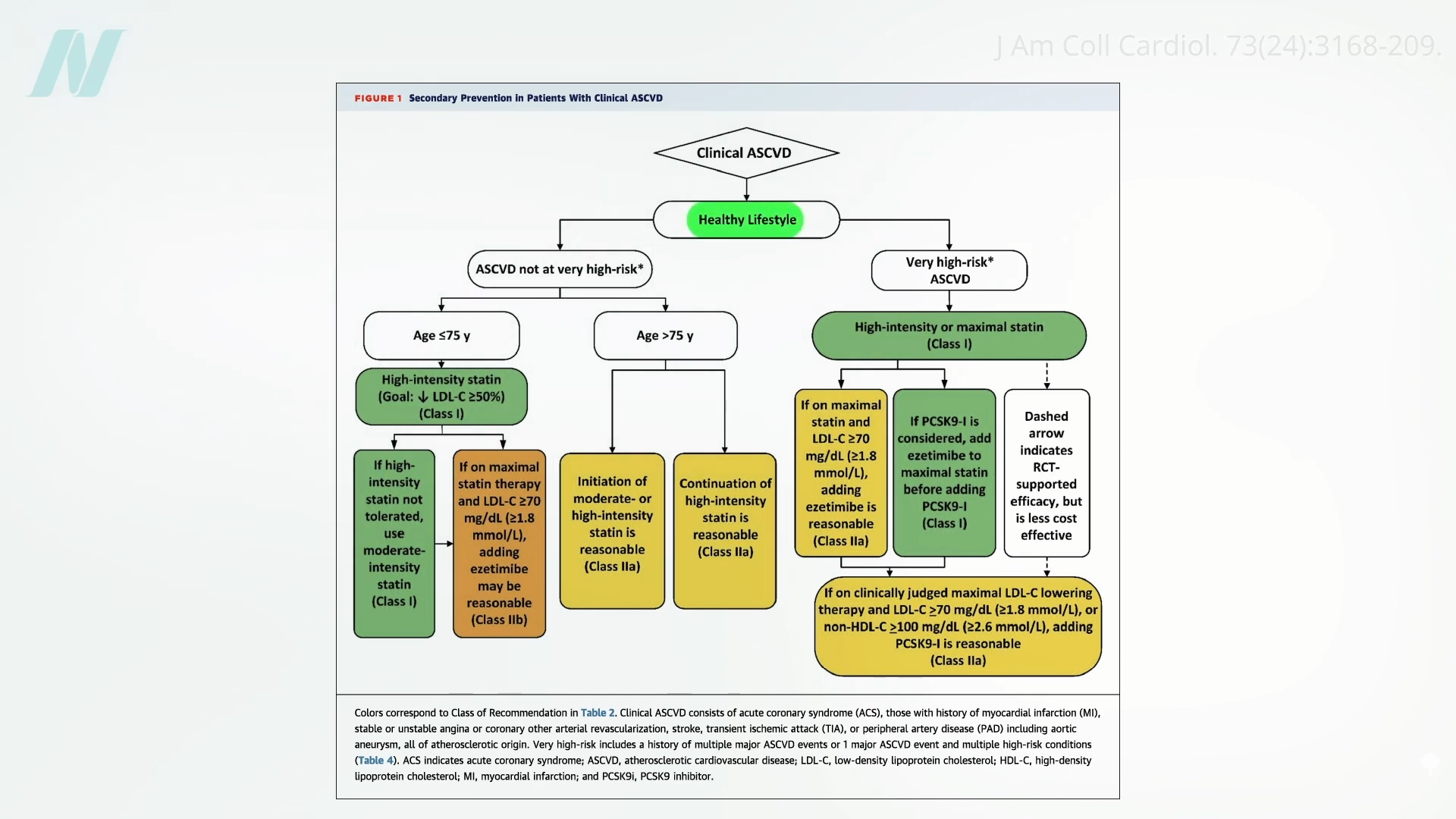
However, clinicians face a fundamental challenge: how can they implement these recommendations without proper nutrition training?
Fewer than 50% of medical schools incorporate any nutrition teaching into their clinical training components. In some cases, the curriculum inadvertently promotes disregard for nutrition, as incoming students generally hold a higher regard for its importance in health compared to when they graduate. Upon entering medical school, roughly 75% of students across various institutions view nutrition as crucial to their future professions. After two years of preclinical coursework, this perception drops sharply-in many programs, it declines to zero percent. Rather than gaining knowledge, students experience a erosion of their initial understanding of nutrition’s value. This preclinical phase effectively diminishes appreciation for practical nutrition applications.
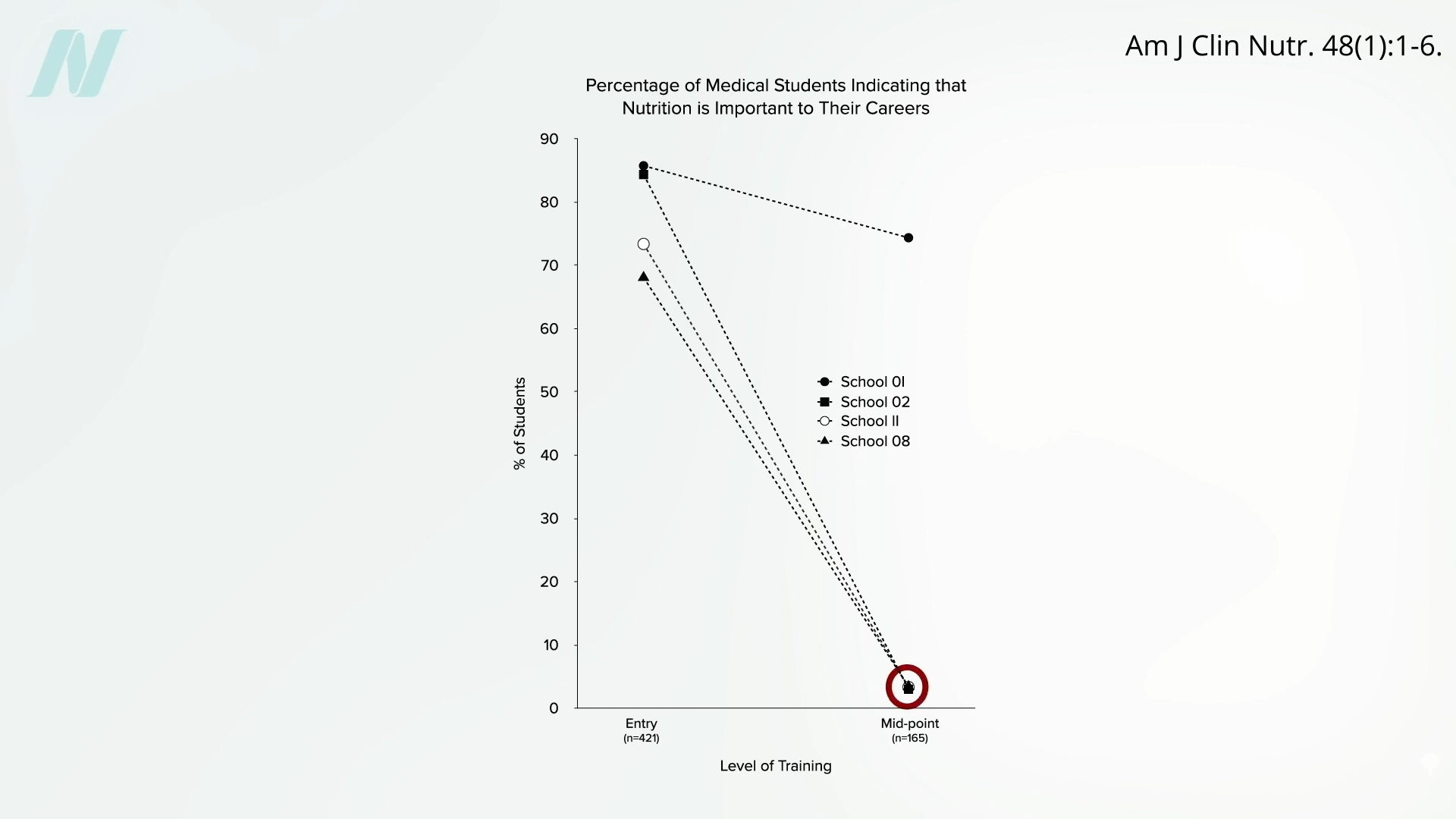
Post-medical school, during residency programs, nutrition instruction remains scarce or entirely omitted. Even recent 2018 updates to residency and fellowship standards included no mandates for nutrition education. Consequently, a resident completing a top-tier internal medicine program might emerge with zero knowledge of nutrition.
What explains the persistent neglect of diet in medical curricula and clinical routines, and how can this be rectified? Among the factors contributing to this oversight is the absence of economic motivations to prioritize nutrition. To counter this, experts from the Food Law and Policy Clinic at Harvard Law School outlined more than a dozen policy strategies spanning every phase of medical training, offering actionable recommendations for policymakers.
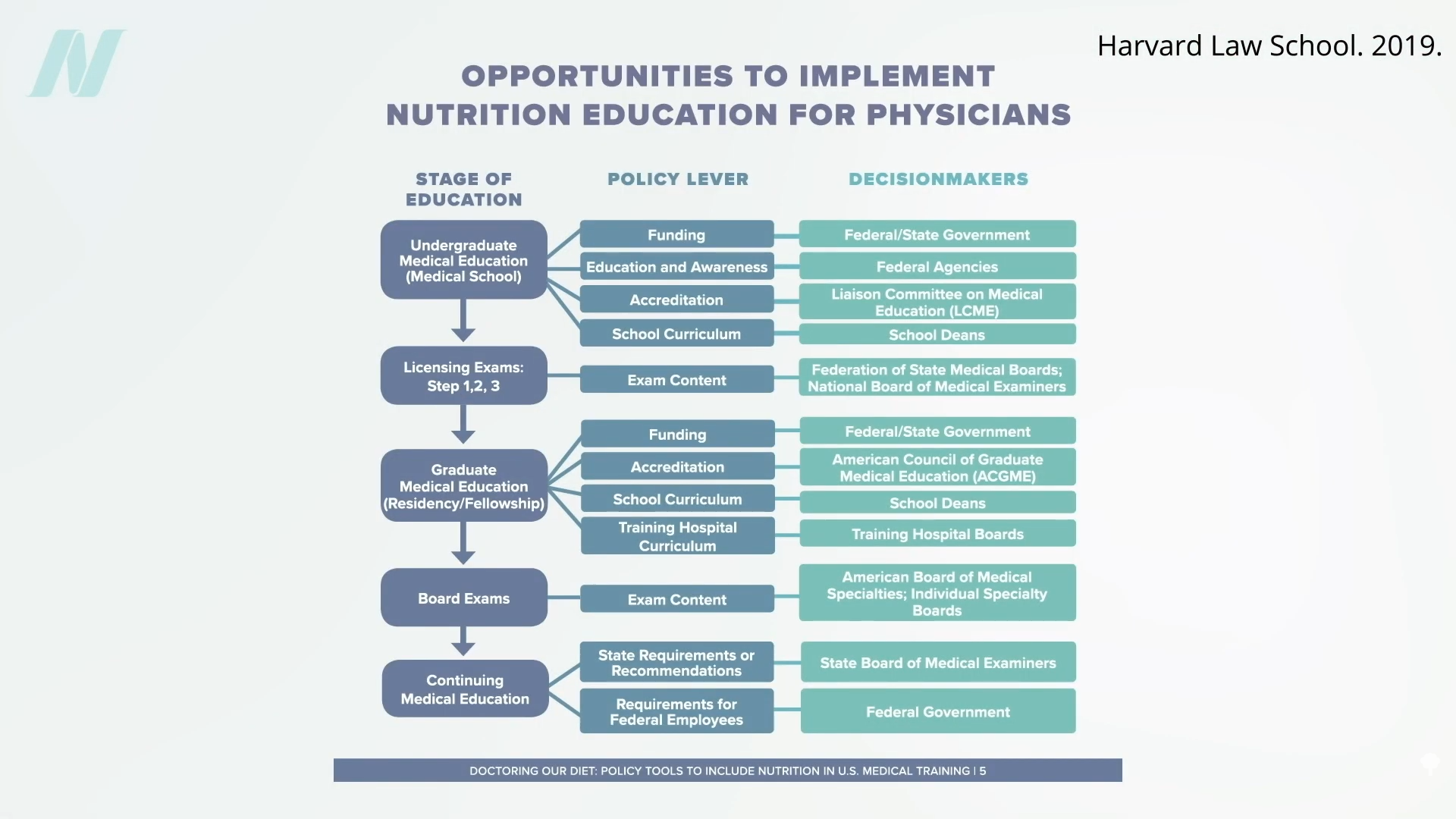
Examples include mandating nutrition coursework for physicians in the Veterans Affairs system or integrating nutrition-related questions into licensing board examinations, thereby compelling schools to prioritize the subject. Currently, even individuals who have recently suffered a heart attack often fail to adopt healthier eating habits post-discharge. This may stem from physicians not emphasizing dietary shifts or from hospital cafeterias serving meals that counteract recovery efforts.
Encouragingly, the American Medical Association has taken a proactive step by approving a resolution that promotes healthier eating environments in healthcare facilities. The resolution urges U.S. health care institutions to enhance wellness for patients, employees, and guests through specific measures: offering diverse healthy options such as plant-based dishes low in saturated fats, trans fats, sodium, and added sugars; removing processed meats from all menus; and prioritizing nutritious beverage choices.
In a parallel development, California enacted a 2018 law requiring hospitals to make plant-based meals available to patients. Several facilities have gone further, including those in Gainesville and Tampa in Florida, the Bronx, Manhattan, and Denver, where dedicated 100% plant-based menus are offered alongside educational resources explaining how plant-forward diets can mitigate chronic conditions.
Examining these innovative menus reveals appealing options like lentil Bolognese pasta, a breakfast featuring cauliflower scramble paired with crispy baked hash browns, mushroom ragu for midday meals, and evening dishes such as hearty white bean stew accompanied by fresh salads and seasonal fruit. These selections represent a refreshing departure from typical hospital fare, actually sparking appetite rather than dread.
The success of these menu overhauls hinged on dedicated physician champions who educated staff and patients about the advantages of plant-rich eating patterns. A lone clinician, armed with scientific evidence, possesses the influence to drive systemic improvements. Physicians occupy a distinctive societal role, enabling them to shape policies from local to national levels-it’s high time this authority is leveraged for nutritional progress.
Key Takeaways
- Although suboptimal diets cause more deaths worldwide than any other factor, medical education provides woefully inadequate nutrition training, often focusing on outdated or irrelevant topics rather than practical patient care needs.
- Students commonly arrive at medical school recognizing nutrition’s vital role but emerge with diminished enthusiasm, as surveys indicate a sharp drop-sometimes to zero-in the proportion viewing it as career-essential.
- Financial disincentives hinder progress, but viable policy interventions include adding nutrition to certification exams and enforcing training requirements for government-employed doctors like those in the VA system.
- Progressive hospitals and state initiatives, including AMA-backed resolutions, are fostering healthier foodscapes by introducing plant-based menus and eliminating harmful items in medical environments.






