An early, uncontrolled study that was never formally published suggested that fasting might offer some positive outcomes for individuals dealing with migraine headaches. However, evidence points in the opposite direction, indicating that fasting could actually provoke migraines more often than it alleviates them. Skipping meals stands out as one of the most frequently reported dietary factors that consistently trigger headaches across various studies and patient reports.
In a comprehensive analysis of hundreds of fasting experiences conducted at the TrueNorth Health Center located in California, researchers observed that headaches occurred in nearly one out of every three participants during their fasting periods. Despite this, the same center documented an extraordinary case involving post-traumatic headaches, which provides intriguing insights into alternative approaches.
According to estimates from the United States Centers for Disease Control and Prevention, over one million individuals in the country experience traumatic brain injuries each year. A prevalent and persistent issue following these injuries is chronic pain, which impacts approximately three-quarters of survivors. Medical interventions for post-traumatic headaches typically begin with pharmaceutical options. When medications prove ineffective, surgical procedures, such as severing specific nerves in the head to interrupt pain signals, become considerations.
But what role might fasting combined with plant-based nutrition play in addressing these conditions? Consider the case of a 52-year-old woman who sought treatment for an intensely debilitating, persistent chronic post-traumatic headache that had plagued her for 16 long years, resisting all conventional management strategies. Remarkably, she found sustained relief through a regimen that started with fasting and transitioned into a diet composed entirely of plant foods, excluding any added sugars, oils, or salt.
Prior to embarking on this path, she had cycled through numerous medications-one after another-with absolutely no success, enduring unrelenting agony day after day for years on end. At the outset, before initiating the fast, her pain was constant and severe. Following the fasting period, the overall intensity of her discomfort diminished by half. Although daily headaches persisted, she began to enjoy intervals completely free from pain. Encouraged by this progress, six months later, she repeated the process. Over time, her headaches evolved into mild episodes lasting under ten minutes and occurring only sporadically. This improvement held steady for months and even extended into years.

Naturally, separating the specific contributions of the fasting phase from the long-term adoption of a whole food, plant-based diet presents challenges, as the two interventions were closely linked in her treatment journey. We are familiar with analgesics, which are substances designed to relieve pain. Conversely, certain foods can act in a pro-algesic manner, exacerbating discomfort. Foods rich in arachidonic acid-commonly found in meats, dairy products, and eggs-fall into this category, as the body converts arachidonic acid into various pro-inflammatory substances that can heighten pain sensitivity.
Shifting to a predominantly plant-based eating pattern effectively reduces arachidonic acid intake, potentially mitigating inflammation-related pain pathways. Many plant foods are naturally abundant in anti-inflammatory compounds, which could further enhance these benefits. In the context of this fasting case, the subsequent plant-based diet likely amplified the initial improvements. When it comes to migraines specifically, increasing plant food consumption while decreasing animal-derived products shows promise, but rigorous scientific testing is essential to confirm these effects.
To explore this hypothesis, scientists conducted a randomized, controlled crossover trial involving individuals who suffered from recurrent migraines. Participants were assigned to either follow a strictly plant-based diet or receive a placebo pill, after which the groups swapped interventions. During the placebo period, about half of the participants reported some improvement in their pain levels, while the other half experienced no change or even worsening symptoms.
In stark contrast, when participants adhered to the plant-based diet phase, nearly everyone noticed substantial enhancements in their condition. This dramatic shift underscores the potential power of dietary interventions in managing migraine symptoms effectively.
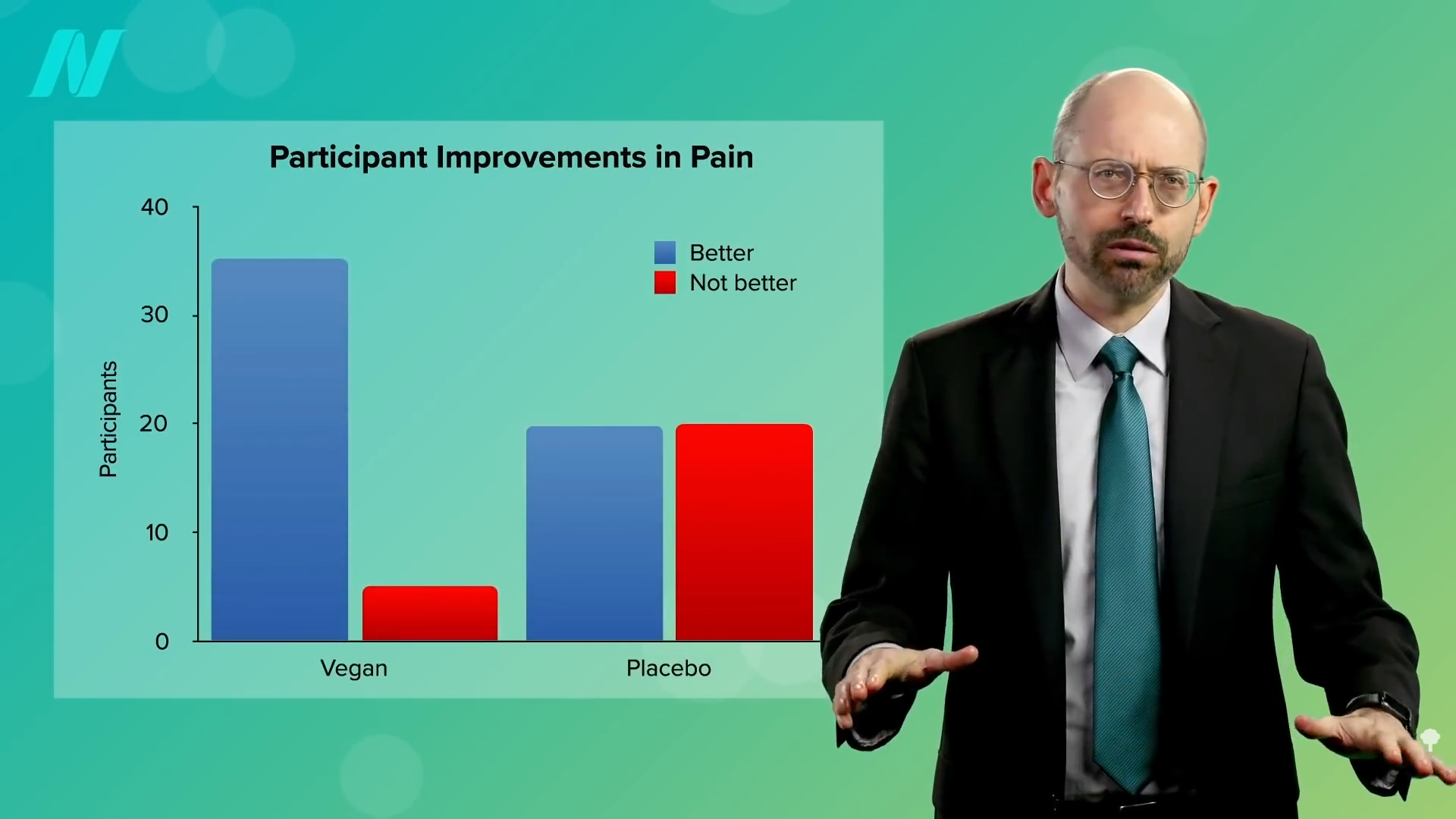
The group following the plant-based diet during the initial phase achieved statistically significant reductions in several key areas: the total number of headaches experienced, the severity of pain during attacks, the number of days affected by headaches, and even the quantity of pain-relieving medications required. The intervention proved so effective that it created an unintended complication for the study design. A substantial number of participants became so reluctant to revert to their prior eating habits after tasting the benefits of the plant-based approach that they opted out of completing the full crossover protocol.
This reluctance is not unique to this trial. Similar patterns have emerged in other research exploring plant-based diets, where participants report feeling markedly better-often dramatically so-and consequently resist returning to their baseline diets. This phenomenon can inadvertently undermine the scientific rigor of such studies by reducing sample sizes or introducing bias, yet it speaks volumes about the real-world appeal and efficacy of these dietary shifts. Plant-based eating patterns, in some instances, deliver results that are almost too compelling to ignore.
Delving deeper into the nuances of fasting’s relationship with headaches reveals a complex picture. While anecdotal reports and preliminary observations have touted fasting as a remedy, the data from controlled fasting environments like TrueNorth Health Center paint a different reality. With headache incidence hovering around 33 percent, it’s clear that fasting does not universally soothe but can indeed provoke discomfort, particularly for those prone to meal-skipping as a trigger.
The post-traumatic headache case stands as a beacon of hope amid this mixed evidence. For this patient, 16 years of unyielding pain gave way to manageable symptoms through a sequenced approach: initial fasting to reset the system, followed by a nutrient-dense, whole food plant-based regimen that sustained the gains. This diet’s exclusion of added sugars, oils, and salt likely minimized inflammatory triggers while maximizing protective phytonutrients inherent in fruits, vegetables, grains, legumes, and nuts.
Mechanistically, the reduction in arachidonic acid merits special attention. This omega-6 fatty acid, prevalent in animal products, serves as a precursor to eicosanoids-potent mediators of inflammation that can sensitize pain pathways in the brain and nervous system. By eliminating these sources and embracing plants rich in omega-3s and antioxidants, the body shifts toward an anti-inflammatory state, which may explain the observed relief in both chronic post-TBI pain and episodic migraines.
The randomized crossover study provides the gold standard of evidence here, minimizing biases through its design. The near-universal improvement on the plant-based arm-contrasted with the mixed placebo results-highlights diet’s capacity to modulate migraine pathophysiology. Reductions in headache frequency, intensity, duration, and medication reliance all point to multifaceted benefits, likely stemming from stabilized blood sugar, reduced vascular inflammation, and enhanced neurological resilience.
Participant dropout due to satisfaction further validates these findings, echoing experiences from trials on plant-based diets for other conditions like diabetes or heart disease. When interventions yield such palpable improvements, adherence becomes the new challenge, turning potential study limitations into testimonials of efficacy.
For those grappling with migraines or TBI-related headaches, these insights suggest exploring fasting cautiously-perhaps under supervision-and prioritizing a transition to whole food, plant-based nutrition. While not a panacea, the evidence builds a compelling case for dietary strategies as viable, low-risk adjuncts to conventional care, potentially offering relief where drugs and surgery fall short.
Key Takeaways
- Although fasting is sometimes promoted for headache relief, evidence shows skipped meals frequently trigger them, with about one in three fasters at a health center experiencing headaches.
- A compelling case report detailed a woman enduring 16 years of severe post-traumatic headaches who gained lasting remission via fasting followed by a strict whole food plant-based diet without added sugar, oil, or salt.
- In a rigorous randomized crossover trial, a plant-based diet dramatically cut migraine occurrences, severity, and medication needs, leading many participants to refuse resuming their prior diets and thus impacting study completion.